Physio Hub:
Evidence-Based Article
Plantar Fasciitis: Why Your Heel Hurts — and How to Fix It Safely
Plantar fasciitis is one of the most common causes of heel and arch pain. It often feels like a sharp, stabbing sensation at the bottom of the foot — especially during the first few steps in the morning or after long periods of sitting.
The good news?
Most cases improve with simple, consistent self-management.
Here’s what plantar fasciitis really is and what you can do today to start feeling better.
What Is Plantar Fasciitis?
The plantar fascia is a thick band of tissue that connects your heel to your toes. Its job is to support the arch and help your foot absorb load during walking and running.
Plantar fasciitis occurs when this tissue becomes irritated from:
-
overuse
-
long periods of standing
-
sudden increases in activity
-
unsupportive footwear
-
foot mechanics like flat feet or high arches
Morning pain happens because the plantar fascia tightens overnight. Your first steps stretch it quickly, causing irritation.
What Actually Helps?
Evidence-Based Self-Management**
1. Reduce aggravating activity — briefly, not completely
Too much rest slows recovery.
Too much loading increases irritation.
A good rule:
Reduce painful high-impact activities for 1–2 weeks, but keep walking and moving.
2. Use supportive footwear
Shoes with:
-
good arch support
-
cushioning under the heel
-
slight heel-to-toe drop
help reduce strain on the irritated tissue.
Avoid:
-
very flat shoes
-
old, worn-out shoes
-
walking barefoot on hard floors (early in recovery)
Heel cups or soft orthotic inserts can also help reduce pain.
3. Do daily stretching — especially in the morning
The most supported treatments for plantar fasciitis are stretches for:
✔ Calf muscles
Stand facing a wall, keep the heel down, lean forward.
✔ Plantar fascia-specific stretch
Sit, cross your affected leg over the other, pull the toes back toward the shin.
✔ Towel stretch before getting out of bed
Hook a towel around the toes, gently pull.
Do these 2–3 times per day. Consistency matters more than intensity.
4. Strengthen gradually
Once pain decreases, strengthening helps prevent recurrence.
Examples:
-
heel raises
-
towel curls
-
short-foot exercises
-
balance drills
The goal is to improve load tolerance over time.
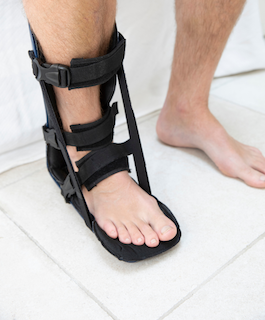
5. Consider a night splint if morning pain is severe
Night splints keep the foot in a gently stretched position.
Research shows they can reduce morning pain in stubborn cases.
What About Ice, Heat, Massage, and Ultrasound?
-
Ice: Helpful for short-term pain relief
-
Heat: Not a first-line treatment; may increase irritation
-
Massage / ball rolling: Feels good but doesn’t fix the underlying issue
-
Ultrasound: Limited evidence for benefit (not essential)
These can supplement your plan, but the cornerstone remains stretching, supportive footwear, and gradual loading.
When Should You See a Professional?
Seek help if:
-
pain lasts longer than 6–8 weeks
-
walking becomes very difficult
-
symptoms worsen over time
-
you have diabetes or numbness in the feet
Physical therapists can provide tailored loading plans, manual therapy, and guidance on footwear and activity modification.
Bottom Line
Plantar fasciitis is painful but very treatable.
Most people recover with:
-
consistent stretching
-
supportive shoes
-
gradual strengthening
-
smart activity modification
With daily care, most cases improve within weeks — not months.
Recommendation by Our Experts
✔ Start your morning with a gentle plantar fascia stretch
✔ Wear supportive, cushioned shoes — especially on hard floors
✔ Add calf and foot strengthening once pain improves
✔ Be patient: consistency beats intensity
< Reference >
- Buchbinder R. Plantar Fasciitis. N Engl J Med. 2004;350(21):2159-2166. doi:10.1056/NEJMcp032745
- Hossain M, Makwana N. “Not Plantar Fasciitis”: the differential diagnosis and management of heel pain syndrome. Orthop Trauma. 2011;25(3):198-206. doi:10.1016/j.mporth.2011.02.003
- Gibbon WW, Long G. Ultrasound of the plantar aponeurosis (fascia). Skeletal Radiol. 1999;28(1):21-26. doi:10.1007/s002560050467
- Riddle DL, Pulisic M, Pidcoe P, Johnson RE. RISK FACTORS FOR PLANTAR FASCIITIS: A MATCHED CASE-CONTROL STUDY. J Bone Jt Surg-Am Vol. 2003;85(5):872-877. doi:10.2106/00004623-200305000-00015
- van Leeuwen KDB, Rogers J, Winzenberg T, van Middelkoop M. Higher body mass index is associated with plantar fasciopathy/‘plantar fasciitis’: systematic review and meta-analysis of various clinical and imaging risk factors. Br J Sports Med. 2016;50(16):972-981. doi:10.1136/bjsports-2015-094695
- Lopes AD, Hespanhol LC, Yeung SS, Costa LOP. What are the Main Running-Related Musculoskeletal Injuries?: A Systematic Review. Sports Med. 2012;42(10):891-905. doi:10.1007/BF03262301
- Menz HB, Thomas MJ, Marshall M, et al. Coexistence of plantar calcaneal spurs and plantar fascial thickening in individuals with plantar heel pain. Rheumatology. 2019;58(2):237-245. doi:10.1093/rheumatology/key266
- Moroney PJ, O’Neill BJ, Khan-Bhambro K, O’Flanagan SJ, Keogh P, Kenny PJ. The Conundrum of Calcaneal Spurs: Do They Matter? Foot Ankle Spec. 2014;7(2):95-101. doi:10.1177/1938640013516792
- Jessup RL, Oates MJ, Johnston RV, Buchbinder R. Shockwave therapy for plantar heel pain (plantar fasciitis). Cochrane Musculoskeletal Group, ed. Cochrane Database Syst Rev. Published online November 25, 2019. doi:10.1002/14651858.CD013490
- Lemont H, Ammirati KM, Usen N. Plantar Fasciitis. J Am Podiatr Med Assoc. 2003;93(3):234-237. doi:10.7547/87507315-93-3-23411.
- Morrissey D, Cotchett M, Said J’Bari A, et al. Management of plantar heel pain: a best practice guide informed by a systematic review, expert clinical reasoning and patient values. Br J Sports Med. 2021;55(19):1106-1118. doi:10.1136/bjsports-2019-101970