Physio Hub:
Evidence-Based Article
Do Ligaments Really Heal?
Why Ligament Injuries Often Recover Slowly—and Incompletely
“You tore a ligament. Ligaments don’t really heal.”
This statement is still commonly heard in clinics and gyms. Ligaments do have limited blood supply, but does that mean they cannot heal at all?
The science tells a more complex story:
👉 Ligaments can heal — but often imperfectly, slowly, and incompletely.
Understanding how and how well ligaments heal is essential for setting realistic rehab expectations and preventing reinjury.
Why Ligament Healing Is So Challenging
Ligaments connect bone to bone and provide joint stability. Compared to muscles, they have:
- Lower blood supply
- Lower metabolic activity
- Fewer regenerative cells
According to Brown et al. (2016), tendon and ligament tissues have poor intrinsic healing potential, and even when healing occurs, it is often structurally incomplete.
This doesn’t mean ligaments never heal — it means the tissue that forms is often:
- Less organized
- Less stiff
- Less resilient to load
What Does the Research Show About Healing Rates?
Healing Does Occur — But Rates Are Low
★ Elbow Ligaments
A longitudinal MRI study by Abehsera et al. (2019) followed patients after elbow dislocation:
- Only 18–41% of injured elbow ligaments showed healing at 2 months
- Many ligaments remained disrupted on imaging
- Clinical function improved despite limited structural healing
👉 Symptoms can improve without full ligament restoration
★ Knee Anterolateral Ligament (ALL)
In a detailed serial MRI study, Saithna et al. (2021) tracked ligament healing for 12 months after ACL reconstruction:
- Only 30.3% of ALL injuries showed full healing by 12 months
- No additional healing occurred beyond 12 months
- Complete tears almost never fully healed
- Healing took >6 months when it occurred
👉 Some ligaments have extremely limited intrinsic healing capacity
How Ligaments Heal (When They Do)
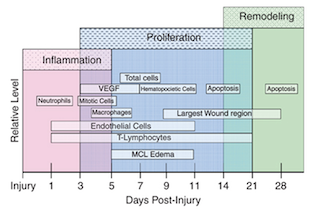
According to Leong et al. (2020), ligament healing follows three biological phases:
- Inflammatory phase – clot formation and cellular signaling
- Proliferative phase – collagen production and fibroblast activity
- Remodeling phase – gradual reorganization of tissue
The problem?
- Collagen alignment is often disorganized
- Mechanical strength rarely returns to pre-injury levels
- The healed ligament may remain more lax and injury-prone
This explains why reinjury risk stays elevated even after “successful” rehab.
Why You Can Feel Better Without Full Healing
One important finding from ligament research is this:
👉 Structural healing and functional recovery are not the same thing.
Studies show:
- Pain reduction does not guarantee ligament restoration
- Neuromuscular control and strength can compensate for tissue deficits
- Rehab can restore function even when imaging looks poor
This is why many athletes return to sport without their ligaments ever fully healing.
What This Means for Athletes and Rehab
- Ligaments are slow to heal
- Healing is often partial
- Tissue quality may never fully normalize
That’s why modern rehab focuses on:
- Progressive loading
- Strength and motor control
- Joint stability through muscles
- Movement quality, not just tissue repair
Researchers increasingly emphasize the need for:
- Advanced regenerative strategies
- Better patient selection
- Combined biological + mechanical approaches
Conclusion: Ligaments Do Heal — Just Not Perfectly
So, is it true that ligaments don’t heal?
❌ Not entirely
✅ But healing is limited, slow, and often incomplete
Most ligaments:
- Heal partially
- Form mechanically inferior tissue
- Remain vulnerable without proper rehab
That’s why rehabilitation quality matters more than biology alone.
Ligament healing is real — but it needs time, load management, and intelligent training to translate into lasting joint stability.
< Recommendation by Our Experts>
✔ Set realistic expectations: ligament healing is slow and often incomplete
✔ Prioritize progressive loading and neuromuscular training
✔ Don’t rely on pain relief alone to judge recovery
✔ Strong ligaments matter — but strong movement systems matter more.
< Reference >
- Brown, Michael N., Brian J. Shiple, and Michael Scarpone. “Regenerative Approaches to Tendon and Ligament Conditions.” Physical Medicine and Rehabilitation Clinics of North America 27, no. 4 (2016): 941–84. https://doi.org/10.1016/j.pmr.2016.07.003.
- Abehsera, Eric, Elvire Guerre, Pauline Duriez, Mazen El Rafei, Christian Fontaine, and Christophe Chantelot. “Ligaments Injuries Check-up and Assessment of Their Healing Potential in Simple Posterolateral Elbow Dislocation: About 25 Cases.” European Journal of Orthopaedic Surgery & Traumatology 29, no. 4 (2019): 785–92. https://doi.org/10.1007/s00590-019-02374-x.
- Saithna, Adnan, Camilo Partezani Helito, Thais Dutra Vieira, Bertrand Sonnery-Cottet, and Koichi Muramatsu. “The Anterolateral Ligament Has Limited Intrinsic Healing Potential: A Serial, 3-Dimensional–Magnetic Resonance Imaging Study of Anterior Cruciate Ligament–Injured Knees From the SANTI Study Group.” The American Journal of Sports Medicine 49, no. 8 (2021): 2125–35. https://doi.org/10.1177/03635465211013015.
- Leong, Natalie L., Jamie L. Kator, Thomas L. Clemens, Aaron James, Motomi Enamoto‐Iwamoto, and Jie Jiang. “Tendon and Ligament Healing and Current Approaches to Tendon and Ligament Regeneration.” Journal of Orthopaedic Research 38, no. 1 (2020): 7–12. https://doi.org/10.1002/jor.24475.